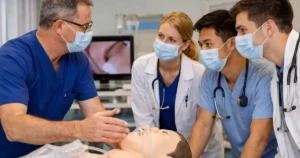
In the ICU, intubation is rarely routine. It happens in unstable patients, under pressure, often with very little physiological reserve.
That is why first pass success intubation matters so much.
Securing the airway on the first attempt is not just a technical goal. It is directly connected to complication rates, patient safety, ICU length of stay, and even hospital resource utilization. When the first attempt succeeds, risk decreases. When it does not, the clinical picture can deteriorate quickly.
What does first pass success intubation mean in critical care
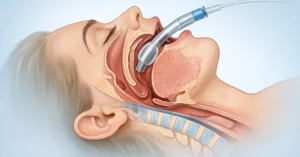
First pass success intubation refers to placing the endotracheal tube correctly into the trachea on the very first attempt without withdrawing and retrying.
Each additional attempt involves:
- Temporary interruption of oxygenation
- Airway manipulation
- Hemodynamic stress
- Increased procedural time
In elective settings, some of this may be tolerated. In critically ill ICU patients, it often is not.
Patients in intensive care frequently present with hypoxia, sepsis, trauma, shock, or cardiac instability. Their margin for error is small.
Why do failed first attempts increase complications
When first pass success is not achieved, complication rates rise significantly.
Oxygen saturation can drop rapidly during repeated attempts. Hypotension may worsen. The risk of aspiration increases. Airway trauma becomes more likely. In the most fragile patients, repeated hypoxia and instability can contribute to cardiac arrest.
Multiple studies in emergency and ICU airway management consistently show that adverse events increase after the first failed attempt. This is why first pass success intubation has become a central quality indicator in airway management protocols worldwide.
Every additional attempt compounds physiological stress.
The impact on ICU outcomes
The effect of first pass success extends beyond the immediate procedure.
Higher first pass success rates are associated with:
- Lower airway-related complication rates
- Reduced severe hypoxic episodes
- Fewer emergency rescue interventions
- Shorter ICU length of stay
- Improved overall stability during critical interventions
For clinicians, this means safer procedures and fewer cascades of complications. For patient safety committees and administrators, it translates into measurable performance improvement.
Resource utilization and hospital efficiency
There is also a practical operational dimension.
Repeated intubation attempts increase:
- Procedure time
- Medication use
- Staff involvement
- Risk of escalation events
Complications often lead to extended ICU care, additional monitoring, and increased costs.
Improving first pass success intubation supports more predictable workflows and reduces variability in critical care delivery. For procurement teams and hospital leadership, tools that contribute to higher first pass rates have both clinical and economic relevance.
Why visualization quality matters
One of the strongest predictors of first pass success intubation is visualization.
Direct laryngoscopy relies on achieving a clear line of sight to the glottis. In many ICU patients, this is challenging due to anatomy, obesity, trauma, cervical spine precautions, or limited positioning options. When visualization is suboptimal, intubation becomes more difficult. Difficulty increases the time. Time increases risk.
Video laryngoscopy improves airway visualization by projecting a magnified view of the glottic structures onto a screen. Instead of relying purely on alignment, clinicians can see anatomical landmarks more clearly and guide the tube with greater precision. Better visualization supports faster decisions and more accurate placement. That combination directly increases the likelihood of first pass success.
How AstraVue supports first pass success intubation
AstraVue’s video laryngoscope systems are designed to enhance visualization in high-pressure clinical environments such as the ICU. Clear imaging allows clinicians to identify airway structures quickly, even in difficult airway scenarios. The ability to share the airway view on a monitor supports team coordination and supervision during critical procedures.
AstraVue systems also offer reusable, disposable, and hybrid blade options, allowing institutions to align airway practice with infection control policies and operational needs. First pass success intubation is influenced by clinician skill, preparation, and environment. Having reliable visualization technology strengthens that foundation and reduces uncertainty during one of the most time-sensitive interventions in critical care.
Making first pass success a strategic priority
For ICU clinicians, improving first pass success intubation protects vulnerable patients during moments of instability.
For anesthesiologists, it supports precision and control. and for hospital leadership, it improves measurable safety indicators and reduces avoidable complications. Airway management will always carry inherent risk. But improving visualization and standardizing technique can significantly reduce that risk. When the first attempt succeeds, patient safety improves. And in the ICU, that difference matters.