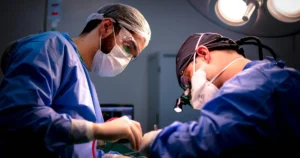
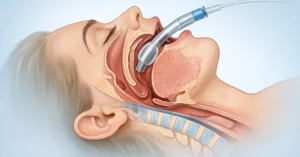
It is early morning in the ICU when a patient with septic shock begins to deteriorate despite escalating oxygen support. Blood pressure is unstable, respiratory effort is failing, and the decision is made to proceed with endotracheal intubation. A junior clinician prepares under supervision. The department recently introduced a new airway device, and although the resident has practiced in simulation, real clinical exposure has been limited.
During the first attempt, the glottic view is not optimal. Minor adjustments are made, but oxygen saturation begins to decline. The supervising physician intervenes, and the tube is successfully placed on the second attempt. The patient stabilizes, yet physiological stress increased during those critical minutes.
Nothing catastrophic occurred. However, this scenario illustrates how variability in experience and familiarity can influence performance during high-risk procedures. This is where intubation training time becomes clinically relevant.
When hospitals talk about intubation performance, they usually focus on first pass success rates, complication rates, and difficult airway protocols. What rarely enters the discussion is something quieter but just as important: intubation training time.
Competence in intubation develops through repetition
Airway management is a procedural skill that integrates anatomical understanding, fine motor control, spatial awareness, and decision-making under pressure. These capabilities do not emerge fully formed after a small number of supervised attempts. They require deliberate practice, progressive exposure to different anatomies, and repeated correction of subtle technical errors.
It is possible for a clinician to demonstrate technical ability while still being early in the learning curve. In such cases, performance may be acceptable under stable conditions but less reliable when stress increases. True proficiency is reflected in consistency across patient types and clinical contexts, particularly when time pressure and physiological instability are present.
For this reason, intubation training time must be viewed as an investment in reliability, not merely as a requirement to achieve minimum competence.
The consequences of compressed or inconsistent training
In busy clinical environments, there is often pressure to accelerate training or assume that once a skill has been demonstrated, it will remain stable. However, airway management skills are sensitive to both frequency of practice and device familiarity. When exposure is limited or inconsistent, variability across operators increases.
That variability may manifest as hesitation during blade positioning, difficulty optimizing the glottic view, or slower advancement of the endotracheal tube. In critically ill patients, even modest delays can contribute to oxygen desaturation or hemodynamic deterioration. Repeated attempts further increase physiological stress and may elevate the risk of complications.
The underlying issue in such situations is not a lack of intelligence or dedication. There is insufficient consolidation of procedural skill. Training time that is too brief, too irregular, or not sufficiently supervised leaves clinicians in a transitional stage of competence where performance may fluctuate.
Workforce dynamics amplify the importance of training time
Modern ICUs operate within complex staffing structures that include rotating residents, cross-departmental airway responsibilities, and varying procedural volumes. In this context, intubation training time becomes a systemic variable rather than an individual one.
When new clinicians enter a department, the speed at which they reach consistent performance affects not only their own confidence but the overall safety profile of the unit. If equipment differs between departments or if visualization systems vary from one setting to another, additional cognitive load is introduced. Each variation requires adaptation, which prolongs the learning curve and increases the potential for inconsistency during early use.
Institutions that recognize these dynamics understand that structured and sustained training is essential for maintaining stable first pass success rates across teams.
The role of visualization in strengthening training quality
Advanced visualization systems have changed the technical landscape of airway management. When a trainee and supervisor can observe the same airway image on a monitor, instruction becomes more precise and immediate. Anatomical landmarks can be identified collaboratively, and corrective guidance can occur before errors compound.
It is important to emphasize that improved visualization does not eliminate the need for thorough training. Rather, it enhances the quality of that training by reducing ambiguity and accelerating pattern recognition. When clinicians repeatedly practice with clear and consistent visualization, confidence develops more efficiently, and performance variability decreases.
This is where the design of airway equipment intersects with educational strategy. The tools used during training influence how effectively the skill is consolidated.
Institutional responsibility and long-term safety
For ICU directors, anesthesia departments, and hospital leadership, the seriousness with which intubation training time is treated reflects the seriousness with which patient safety is regarded. Structured training pathways, regular supervised exposure, and equipment standardization are not optional enhancements. They are foundational elements of safe critical care practice.
AstraVue’s video laryngoscope systems are designed to provide consistent and high-quality visualization in demanding clinical environments. By supporting shared visibility and reliable imaging, they create a setting in which training can occur with clarity and precision. While technology alone does not produce competence, it can strengthen the environment in which competence is built.
A broader perspective on preparation and performance
Intubation success is often evaluated at the moment the tube is secured. However, that moment reflects months of preparation, repetition, and refinement. The stability of a clinician’s performance under pressure is determined long before the procedure begins.
When institutions commit to sufficient intubation training time and align their equipment with structured educational practice, they reduce variability and strengthen first pass success across the department. In critical care, where patients are often at the limits of physiological tolerance, such commitment is not merely operational. It is ethical.