Blade geometry influences technique. Video laryngoscopy influences system behavior.
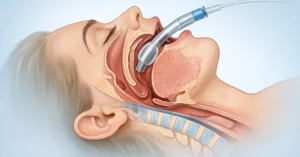
Blade design has always been central to airway management. Macintosh and Miller blades shaped generations of clinicians, and the introduction of hyperangulated and channeled blades expanded options for difficult airways. Blade geometry determines how the airway is approached, how the epiglottis is manipulated, and how the endotracheal tube is advanced. These differences matter at the procedural level.
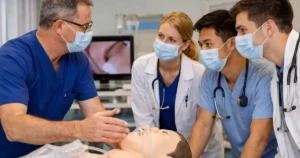
However, the introduction of video laryngoscopy shifted airway management from a purely mechanical act to a visual system. Once intubation moved from direct line of sight to screen-mediated visualization, consistency of the visual interface became a defining factor in performance reliability. Blade variation optimizes anatomy. Video visualization stabilizes interpretation. In a modern ICU, interpretation often matters more than mechanics.
Video laryngoscopy changed more than just the view
With direct laryngoscopy, the blade shape determined both exposure and perspective. With video laryngoscopy, exposure and perspective are partially separated. The camera, screen, optical angle, and image processing now shape how anatomy is perceived.
This shift introduced new advantages, including shared visualization, improved supervision, and better documentation. It also introduced new variables. Screen size, brightness, image lag, distortion, and angle of projection can differ between systems.
When clinicians work within a single, consistent video platform, their visual pattern recognition stabilizes. They learn how the glottis appears on that system and understand how depth perception translates to tube advancement. They develop familiarity with how hyperangulated blades behave on that specific screen. When they frequently switch between platforms, that visual familiarity resets. The blade may be similar. The visual interpretation may not.
ICU variability amplifies the impact of visual inconsistency
Intensive care units rarely operate with a single operator. Residents rotate monthly. Attending physicians supervise intermittently. Emergency and anesthesia teams cross-cover. Devices move between departments.
In this environment, inconsistency in video visualization introduces subtle but cumulative adaptation demands. A clinician who trained on one optical profile may encounter a different contrast curve or projection angle during an emergency intubation. The difference may be minor in isolation, yet under stress, it can influence speed and confidence.
These micro adaptations do not always result in failure. More often, they contribute to variability. Variability influences first pass success. The first pass success influences patient safety. When institutions analyze airway performance metrics, the question should not only be which blade performs best in difficult anatomy. It should also be determined whether the visualization environment remains stable across the team.
Training consolidation depends on visual repetition
Video laryngoscopy has transformed airway training because instructors and trainees share the same view. This shared visualization allows real-time correction and structured feedback. However, the benefit is maximized only when that view remains consistent over time.
If a trainee practices on one video system during simulation but encounters a different one in the ICU, cognitive recalibration occurs. The anatomical landmarks are identical, but their representation differs. The learning curve fragments.
When blade options such as Macintosh, Miller, hyperangulated, and channeled configurations are available within a unified video platform, training becomes layered rather than disrupted. Clinicians can adapt blade choice to anatomy while preserving visual familiarity. This is where video laryngoscopy, when implemented as a coherent system rather than a collection of devices, supports institutional reliability. As discussed in our analysis of intubation training time, repetition only consolidates skill when the visual environment remains stable.
Elevating video laryngoscopy beyond device comparison
The debate between blade shapes is important, but it is incomplete without addressing the platform on which those blades operate. Video laryngoscopy is no longer simply an alternative to direct laryngoscopy. In many ICUs, it has become the primary modality for airway management.
Once video becomes the dominant modality, the consistency of that visual ecosystem becomes a strategic decision. Institutions that standardize their video platform while maintaining appropriate blade diversity may reduce cognitive load, strengthen supervision, and stabilize performance across rotating teams. This is not an argument against blade innovation. It is an argument for platform coherence.
AstraVue’s systems approach
AstraVue’s video laryngoscopy platform offers channeled hyperangulated, hyperangulated, Macintosh, and Miller blades within a unified visualization architecture. This allows clinicians to select the blade best suited to the patient while maintaining consistent optics, screen behavior, and ergonomic familiarity.
The emphasis is not on promoting one blade over another. It is on preserving visual stability across clinical contexts. In high acuity ICU environments, where reliability across operators matters as much as technical optimization, stability can influence overall performance.
Video laryngoscopy is most powerful not when it introduces variation, but when it introduces clarity and consistency.