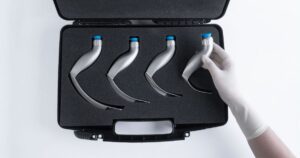
On paper, a low-cost laryngoscope can look like a good deal. It meets basic requirements, fits the budget, and works, at least for a while. But in real clinical settings, where every second and every decision counts, cheap or outdated airway tools often reveal their true cost through patient complications, wasted time, and loss of trust.
This is the hidden cost of traditional laryngoscopes, and it is one that the healthcare industry can no longer afford to ignore.
The traditional laryngoscope: reliable but limited
For decades, direct laryngoscopy was the foundation of airway management. It provided a simple and direct view, relying entirely on the clinician’s skill and line of sight.
In skilled hands, it worked, but not without challenges.
In difficult airways, limited neck mobility, or emergency scenarios, traditional laryngoscopes often fall short. The lack of visualization and reliance on guesswork could increase the risk of multiple intubation attempts, hypoxemia, and trauma.
With the introduction of video laryngoscopes, a new standard emerged. These systems provided a clearer, magnified, and illuminated view, making difficult airways manageable and improving first pass success rates dramatically.
Still, many hospitals and clinics continue to rely on older, low-quality direct systems, unaware of how much those devices are really costing them.
The hidden cost 1: compromised patient safety
Every failed or delayed intubation carries clinical consequences.
Studies from the American Society of Anesthesiologists show that limited visibility is among the leading causes of failed intubation, particularly in emergency and ICU cases.
Low-quality traditional laryngoscopes often contribute to:
- Fogging or glare that obscures the vocal cords
- Poor illumination forces clinicians to reposition repeatedly
- Inconsistent blade curvature that makes insertion less predictable
- Handle instability that disrupts alignment during the procedure
These problems are not just inconvenient. They can lead to oxygen desaturation, airway trauma, or even cardiac arrest during prolonged attempts.
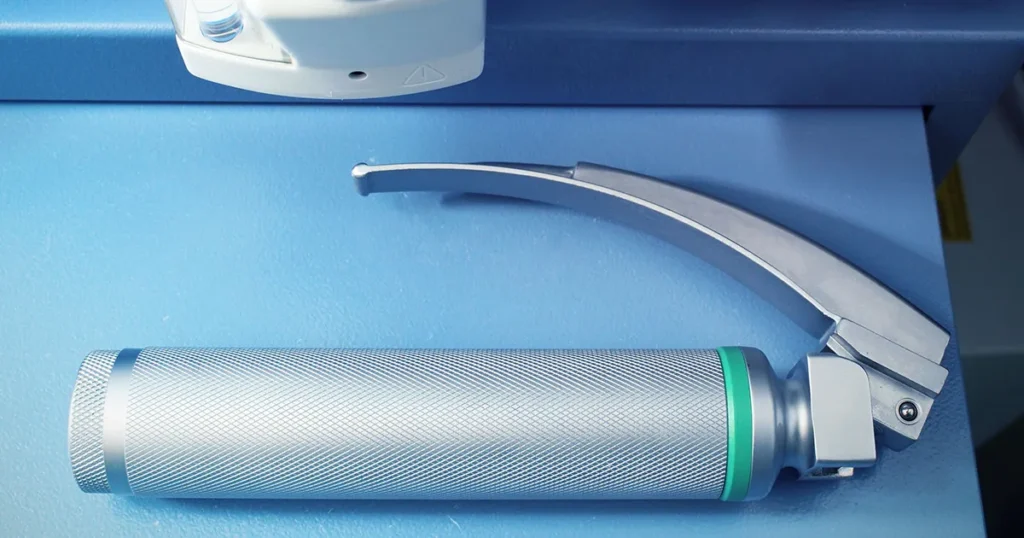
The hidden cost 2: false savings on procurement
The biggest trap for hospitals and distributors is assuming that a cheaper laryngoscope saves money.
In reality, low-cost devices often lead to:
- Frequent replacements due to poor build quality
- Higher maintenance and sterilization costs
- Downtime when equipment fails during high-volume use
- Loss of staff confidence, prompting requests for replacements
- Reusable devices made from surgical-grade stainless steel can last for years when maintained properly. Disposable systems ensure infection-free, consistent performance with no hidden costs of cleaning or reprocessing.
A low upfront price may look appealing, but over time, these hidden expenses quietly surpass the investment in a quality video laryngoscope system.
The hidden cost 3: missed clinical efficiency
When clinicians face repeated failed attempts or poor visibility, procedure times extend, oxygen levels drop, and the stress level in the room rises.
Each extra minute during intubation increases risk.
Each delay impacts workflow, operating room scheduling, and overall patient throughput.
Modern video laryngoscopes solve this by offering real-time HD visualization, faster decision-making, and less operator fatigue. In teaching hospitals, the ability to share the screen helps instructors guide trainees efficiently, improving both learning and safety.

The hidden cost 4: infection risk
Traditional reusable laryngoscopes require rigorous sterilization between procedures.
In practice, incomplete cleaning is one of the most common causes of cross-contamination in airway equipment.
A study published by the Journal of Hospital Infection found that nearly thirty percent of reusable laryngoscope blades retained organic material even after cleaning.
Low-quality devices make this worse:
- Poor surface finishing traps debris and biofilm
- Inconsistent waterproof sealing damages electronics during disinfection
- Weak joints allow bacterial buildup over time
- Modern video laryngoscopes with sealed waterproof components and disposable blades eliminate these risks, supporting infection prevention protocols aligned with World Health Organization recommendations.
The hidden cost 5: lost trust from clinicians and patients
Hospitals that repeatedly experience equipment issues eventually lose something even more valuable than money — trust.
Clinicians want tools that respond the way they expect them to. When a laryngoscope fails to deliver consistent imaging or ergonomic comfort, confidence erodes quickly.
This affects:
- Clinical performance with more time spent troubleshooting
- Staff morale increased with frustration due to unreliable tools
- Patient perception when complications or delays occur during airway management
- Choosing a high-quality, certified system signals commitment to safety, efficiency, and care — values that strengthen both institutional credibility and patient confidence.
The better alternative: quality and reliability with video laryngoscopy
The shift from traditional to video laryngoscopy is not just technological. It is ethical.
When hospitals invest in high-quality video laryngoscopy systems, they are not buying gadgets. They are buying:
- Consistent first pass success rates
- Reduced complication risks
- Fewer reprocessing errors
- Improved clinical teaching and collaboration
AstraVue’s range of reusable, disposable, and hybrid video laryngoscopes combines HD visualization, bright LED lighting, and precision-built components, all tested against international standards including FDA, CE, MDR, and ISO 13485.
The true cost: what hospitals and distributors need to remember
Traditional or low-quality laryngoscopes may look affordable, but their real cost hides in:
- Increased patient complications
- Unplanned replacements and repairs
- Extended procedure times
- Higher sterilization expenses
- Damaged professional trust
AstraVue was built on one principle: precision saves lives.
Every component, from blade design to imaging sensor, is crafted to deliver reliability hospitals can depend on and distributors can stand behind.
When it comes to airway management, the cheapest option is rarely the safest. The smartest investment is one that lasts.